Chronic Pain Doesn’t Heal in Isolation: A Relational View of Pain
Survival strategies, inherited loyalties, and the relational patterns that keep pain alive

If I had to describe the core of my work, I would say this: I work with pain.
This includes pain that lingers without a clear cause, as well as other chronic symptoms that develop in muscles, joints, organs, or connective tissue over time. I also work with emotional and relational pain that people often carry quietly for years, sometimes even decades, while life goes on around them.
Most people deal with pain by managing, ignoring, numbing, or pushing it aside. They adapt and keep moving forward. What many don’t realise is that much of the pain people carry is not only personal, but inherited or absorbed through the relationships and environments they grow up in. Without knowing it, we remain loyal to the pain patterns of our bloodlines and to the emotional climates that shaped us. There can be a strange kind of love in this, one that becomes woven into identity. Often, it’s a love shaped by responsibility, obligation, survival, and adapting to hard situations. This kind of conditional acceptance is common in early relationships, where children learn that connection depends on adapting to the emotional needs of the environment, even when there hasn’t been obvious trauma.
In my work as a psychosomatic integration consultant, I help people reconnect with parts of themselves that were pushed away, held back, or forced to carry too much on their own. When these parts are ignored or overridden for long enough, they often manifest in the body as pain, tension, collapse, or chronic symptoms.
I came to psychosomatic work through lived experience with chronic emotional, physical, relational, and psychic pain, including recurring conditions and symptoms that emerged at key transition points. All this is to say, I am not separate from the patterns I work with. Pain has quietly run through my family for generations—that pattern did not skip me. For extended periods, I managed symptoms by over-functioning, staying focused, engaging socially, or relying on distraction and addiction—anything that kept emotion and vulnerability at a distance. At other times, these symptoms became overwhelming, making it difficult to think clearly, stay organised, or function as usual. This pattern is also common in family systems where pain is carried across generations and remains largely unacknowledged. What is pushed away, unsupported, or unwitnessed does not disappear. It waits, often held in the body, the nervous system, or in parts of the psyche that learned early on to carry what could not be expressed. When that material finally surfaces, it can feel volcanic, destabilising, or confronting, particularly when it has never been met with enough safety or containment. I have also come to notice that pain often shifts during transition, relationship change, relocation, transformation, or solitude.
The patterns I’m describing here appear across class, income, nationality, and life circumstance. While external conditions differ, the internal patterns do not. Pain is not selective. It does not discriminate based on intelligence, success, resources, or social position. It adjusts to each situation and expresses itself in ways that fit the person experiencing it.
Rethinking Chronic Pain
People with chronic pain often come to me feeling confused and frustrated. They have been through tests and medical checks. Sometimes there was an injury. Sometimes there wasn’t. Many have tried medications, physical treatments, or even procedures, and still the pain persists. What they do know is that the pain is still there, and no one has been able to clearly explain why.
This does not mean the pain is imagined or all in your head. The pain is definitely real. In psychosomatic work, persistent chronic pain is understood as a sign that the nervous system is still carrying unresolved stress and unprocessed emotional and relational experience. Over time, that accumulated load settles into the body as chronic tension and activation, which is felt as pain.
The body is always asking, Am I safe? That answer often depends more on lived history than on what’s happening right now. If someone grows up with long-term stress, unpredictability, or emotional tension, their nervous system learns to anticipate danger. And even when things are safe, that alertness can stick around. The body stays tense, and even small sensations can feel bigger. As children, they often noticed small signs from caregivers, like tension in a voice, a change in mood, or conflict in the room, especially in emotionally volatile environments. Over time, their bodies learn to stay on alert and vigilance becomes a baseline setting rather than a temporary response, so present situations can trigger reactions as if earlier danger were still active. Things like a crowded train, a tough conversation at work, or even a mild illness can set off a strong response.
I often see clients whose jaws clench, throats tighten, or stomachs knot during periods of interpersonal stress. Some develop sinus pressure or headaches, even when medical tests show nothing acute is wrong. The muscles and tissues are bracing as if they need to protect the body. So what looks to be a purely physical symptom is also a record of how the nervous system has learned to respond to tension.
At the same time, pain can also emerge when something that was never allowed to take up space begins to surface. This is often seen in people who, as children, were not permitted to express anger, distress, or need. Parts of the system that were silenced or overridden may later show up as pain. Clients sometimes describe this pain as “hot,” “inflamed,” or “screaming.” These bodily descriptions often echo emotional states that were never given permission to exist.
What’s important to understand is that these responses are not inherently disorders, even though they’re often treated that way. Diagnostic labels can be useful because they help organise care, but they can also shrink how we see what’s happening. When we look at a response only as a problem to fix, we can miss that it originally developed as a way to survive. The difficulty comes when life changes but the nervous system keeps relying on the same protective habits. If we treat those habits only as symptoms to get rid of, we risk pushing them down and locking them in place instead of helping them learn something new. Over time, carrying that internal load has consequences. Chronic pain is one of the ways it can show up.
Protective Parts, Inherited Pain, and the Relational Nature of Relief
Many of the behaviours that accompany chronic pain make sense when viewed as survival strategies. Avoiding movement (for example, becoming increasingly sedentary or restricting activity to avoid flare-ups) can be a way to prevent further harm. Staying hyper-alert is the nervous system scanning for danger. Pushing through pain can be tied to self-worth or survival, especially if resting once felt unsafe. Numbing or disconnecting (sometimes experienced as dissociation) often protects against emotions that were once overwhelming or unacceptable.
I often work with people who are very capable and seem successful on the outside, but feel disconnected from their bodies. They handle work, relationships, and responsibilities well, but have trouble sensing their limits, boundaries, or certain emotions. For them, physical sensations can feel either dull or too intense, since staying connected to their bodies once felt unsafe.
If anger, grief, fear, shame, or need could not be safely expressed earlier in life, the body often holds onto those feelings. Pain can become the place where these unprocessed emotions and unspoken boundaries remain. The body is not broken; it has just carried too much for too long without enough support or permission to let go. Sometimes these patterns come from personal history. Sometimes they emerge within relationships. And sometimes they are inherited.
Inherited patterns often appear as quiet loyalties that are easy to miss. This can show up as resistance to success, ease, receptivity, or visibility, even when those things are consciously desired. Becoming the first in a family system to experience stability or freedom can activate internal brakes from a part that equates moving beyond the family’s experience with loss of belonging. In other cases, loyalty forms around suffering itself. Some people repeat patterns they hoped to escape. When love, safety, or recognition were scarce, the system may maintain connection by mirroring the suffering it knows. This is not a conscious choice. It is a nervous system trying to stay bonded in the only way it learned.
From this perspective, pain, repetition, or self-sabotage are attempts to stay connected. The body often chooses belonging over comfort, even when the cost is high.
This tells us something important about the nature of pain itself:
Pain is highly relational. It tends to intensify or soften in response to the quality of contact a person is experiencing in their life.
That includes internal relationships with different parts of the self and external relationships that offer or withhold safety, recognition, and responsiveness. These two are closely linked and often mirror one another. This also helps explain why pain can sometimes shift simply through being met. Many people have noticed that symptoms ease after a medical appointment, a conversation, or a moment of being listened to, even when no new treatment is introduced. What changed was not the body, but the presence of contact. This aspect of pain is central to understanding why relief does not emerge through self-management or medication alone.
Finding Relief Is Relational
One of the most overlooked aspects of chronic pain is that relief rarely happens in isolation. When pain develops in the absence of sufficient contact, or support, it tends to persist until those conditions change. Emotional material that was left alone—grief, rage, shame, loneliness, fear—does not simply fade. Without somewhere to be met, it intensifies and often finds expression through the body.
This is why isolation often amplifies pain. Many people living with chronic pain are highly self-reliant, not by preference but by necessity. Needing others once carried risk, whether through disappointment, conflict, or loss of control, so distance became the safer option. Over time, self-containment becomes habitual.
Without relational safety or opportunities for co-regulation, the nervous system has no external reference point for ease. Everything must be managed internally. And with that, stress accumulates, and pain systems remain active.
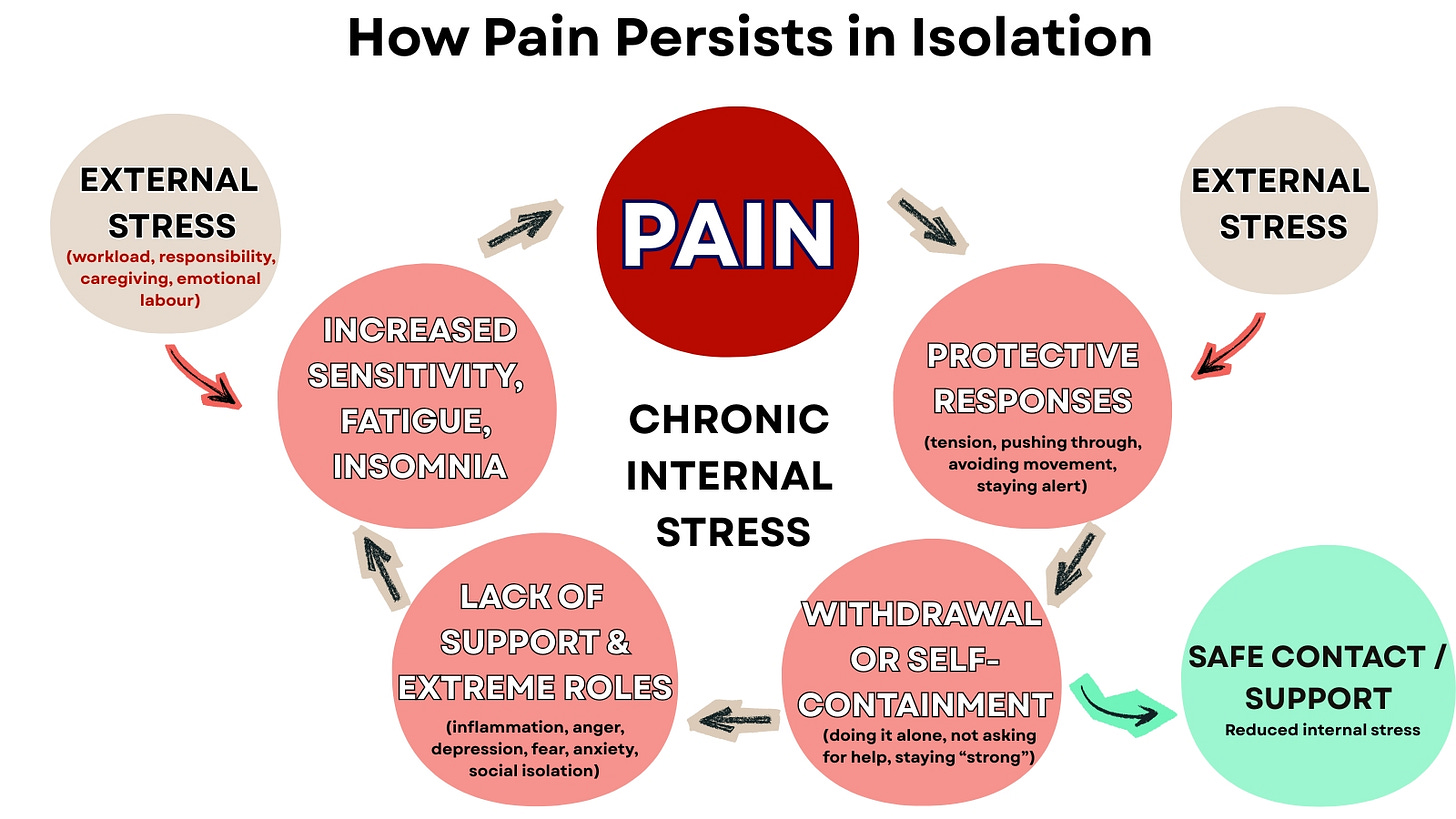
This pattern is especially common among high-functioning adults and those with relational responsibilities, such as leaders, founders, caregivers, and helping professionals like therapists, educators, and facilitators. It also appears in people whose survival strategies focus on managing relationships and threat in different ways. Some become chronic people-pleasers or appeasers, while others cope by trying to control situations, withdrawing, or shutting down emotionally. They often carry disproportionate responsibility in relationships while receiving little support themselves. Even when surrounded by others, the connection often involves giving, managing, controlling, performing, or holding things together rather than being met.
When we don’t have places to rest, feel supported, or be heard, our sensitivity grows, and pain can get worse. Relief often comes not from trying harder, but from safe connections. These connections might be found in relationships, therapy, groups, time in nature, creative activities, spiritual or faith-based practices, or body-based practices such as movement, dance, or gentle somatic disciplines. The important thing is that pain does not have to stay isolated.
Pain often eases when it no longer has to carry everything alone.
Listening to the Body Again
A significant shift in working with chronic pain involves learning to listen to the body again, not as something broken, but as a source of information. Many high-functioning adults are highly attuned to others and skilled at managing situations, yet disconnected from their own internal signals.
Rebuilding this connection happens when there is enough relational safety and trust to feel sensations again. Listening to the body does not mean giving in to symptoms or becoming passive. That fear usually arises from parts that learned early on to keep going at all costs; the internal drive that pushes you to function, perform, and override discomfort. In this work, the nervous system is gradually presented with a different experience: safety without that “keep going” part in control.
This happens through contained, titrated moments of presence, often with someone who can offer regulation. The task is not to analyse, override, fix, or eliminate what arises, but to stay present with it long enough for the system to register that it is no longer alone and no longer under threat. In practical terms, this can look like allowing yourself to fall apart in the presence of someone who doesn’t rush to organise or minimise the experience, but stays with you and treats your state as a valid response. Over time, this changes how pain is experienced, because the parts holding it are no longer carrying it in isolation, but are being met in relationship.
It can be difficult to fully understand this process just by thinking about it. Information can help describe what is happening, but it does not replace actually experiencing it in relationship. The work often feels slow and ordinary at first. It usually involves staying present with what is happening at a sensation level in the body, rather than immediately moving into story, analysis, or problem-solving. That shift — from thinking about experience to feeling it directly — can be uncomfortable, especially for people who are used to moving quickly, working cognitively, and solving problems through strategy or intellect.
This shifts the emphasis away from constant action and toward tolerating experience. It asks for less doing and more allowing. Less managing. Less holding things together. Less being useful to others. For many people, this is the missing experience. Being met as they are, without having to perform, explain, help, or carry responsibility, is often what the pain has been pointing toward all along.
Where This Connects to My Work
This is where I use the Psychosomatic Restoration™ Method in my work. This method is focused on supporting our parts that have held grief, anger, fear, shame, responsibility, and unspoken boundaries. Through nervous system regulation, attachment-based relational work, and parts integration, the system begins to reorganise. Old protective strategies are no longer forced to run the show. As Nancy Sowell, LICSW (IFS Institute) describes, healing emerges through ‘non-anxious relationship’. When the system is met without urgency, pressure, or agenda, it begins to update. What once had to be contained can move. What once had to be managed can be felt. What once showed up as pain can change form.
This is the core of my work: helping people change old relationship patterns, reshape their nervous system, and support those who are ready to move beyond just surviving. The goal is not to push the pain away, but to create conditions in which it no longer has to shout for attention.

